A recent Nature article, by Dr Donna Farber of Columbia University in New York, has highlighted how utilizing human tissues can improve our understanding of disease pathology1 — particularly when those diseases involve the human immune system. Dr Farber detailed the complexity of human immunity, describing how immune cell populations can vary from one tissue to the next, and how studies in human tissues have led to the development of novel immunotherapies for cancer and arthritis.
The professor cited the work her team carried out during the COVID19 pandemic2 as an example. When studying the immune cells in airway samples from COVID-19 patients, she noted unusual cell-surface receptor and cytokine expression. By comparing this immune population to the corresponding blood samples, her team discovered that monocytes in the blood were being recruited and altered by cytokines produced by the airway. This is just one example of how human tissue research can be a powerful alternative to conventional models; even living animal models where species differences are also apparent.
Inter-patient studies using human tissue
The power of human fresh tissue testing is a phenomenon scientists at REPROCELL (formerly Biopta) have observed for many years. Since 2002, they have been developing innovative ex vivo models using human living tissues, transported straight from consented patients to their laboratories in Glasgow, UK, and Maryland, USA. When the co-founder of Biopta, Dr David Bunton, started working with human tissues it was clear that their translational capability was superior to other pre-clinical models. Not only did these functional human tissues display the inter-patient variation that is observed naturally in the human population, but they could be used to compare directly with animal or clinical data to troubleshoot adverse effects or prove efficacy in humans, rescuing compounds from clinical failure. To date, REPROCELL has conducted over 1,000 projects for Pharma and Biotech companies to assess the safety, efficacy or bioavailability of novel drugs in human “living” tissues, and has generated numerous publications with Pharma.
As described in the Nature paper, a current trend is towards the use of fresh tissues obtained from patients with inflammatory or auto-immune conditions; such as gastrointestinal biopsies obtained from patients with inflammatory bowel disease, or skin biopsies from patients with psoriasis. Using fresh tissue derived from the target patient group allows a deeper understanding of the complex three-dimensional and multicellular response in a system that more closely reflects the interaction of cell types.
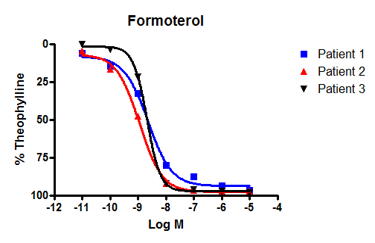
This unique ability to mimic patient variation pre-clinically is demonstrated below (figure 1). In this study, REPROCELL scientists isolated functional airways from lungs not suitable for transplant, from three organ donors and measured their response to the known bronchodilator drugs, formoterol, and salmeterol.
Whilst all of the patient tissues responded equally to formoterol, there was a significant difference in their responses to salmeterol. This same phenomenon is observed clinically: physicians who prescribe salmeterol inhalers often find that patients do not respond equally to this drug as they do with formoterol. What is even more interesting about this data is that it shows a clear responder, high-responder, and low-responder to salmeterol (patients 1, 2, and 3 respectively).
A
B
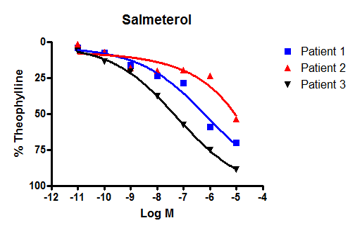
Figure 1: Bronchodilation of human isolated airways in response to increasing concentrations of beta-adrenoceptor agonists. A: All donors responded equally to formoterol. B: By contrast, only patient 3 (red line) and 2 (blue line) responded to salmeterol - patient 1 (black line) was a poor responder. Differences in the response to salmeterol are explained by variations in patient genotype that affect β-adrenoceptor sensitivity.
This ability to harness inter-patient variation for precision medicine was demonstrated by REPROCELL in 2019 when the company published data showing how human living tissue research could aid precision medicine strategies3. Using lung samples from 25 COPD patients, researchers identified two genes that could be responsible for inter-individual differences in drug response. Not only did this study identify potential new targets for COPD treatments, but it also demonstrated that human tissues have the potential to be used to stratify patient populations prior to clinical trials, thereby making the trial much more likely to succeed in the defined patient subset. You can find out more about the methodology behind the early stratification of your target population here.
Obstacles to human tissue research
Another important point highlighted by Dr Farber is that there are regulatory and logistical obstacles that are blocking the widespread use of human tissue research. She recommends the promotion of paired sampling, such as autologous airway and blood samples, like those used in her COVID-19 study. She also points out that in addition to blood and serum samples, more biobanks should stock frozen tissues and secretions, which are rich in immune cells and soluble factors (you can browse our wide range of frozen human tissue samples here).
Yet perhaps most interestingly, she emphasizes the importance of collaboration in human tissue research. Anyone who has ever attempted to use human tissues in their research will recognize the ethical and logistical barriers. Human tissue testing requires a vast range of knowledge from both a regulatory and technical perspective which can be intimidating to approach alone. At REPROCELL we are experts in this area and have developed and expanded our tissue networks and ethical and regulatory knowledge over the past 20 years. With increased interest in the area of precision medicine, human tissue studies are likely to become larger and more collaborative. For example, REPROCELL's 2019 precision medicine exemplar project and publication3 involved individuals from a variety of areas, including academia, industry, medicine, and digital technology.
Outsourcing human tissue testing
Due to the barriers, Dr Farber highlighted in accessing human tissues, many scientists choose to outsource human tissue testing to specialist contract research organizations such as REPROCELL. For two decades, REPROCELL has been providing human tissue testing services to leaders in Biotech and Pharma, acting as their "Human tissue research department". In our laboratories, scientists are on call 24 hours a day to accept human fresh tissues as soon as they are made available. The freshness and functionality of these tissues are key to the translatability of these models, so all tissues undergo a functional validation process and are rejected if they fail these quality control tests.
This dedication to sourcing and utilizing fresh human tissues for precision medicine applications is why REPROCELL has worked with 24 of the top 25 pharma companies globally. REPROCELL is now planning to partner with innovative pharma companies in the development of new precision medicine strategies. By providing patient stratification at an early stage and following this through to the clinic, human tissue testing could ensure that future treatments are more effective than ever.
Further reading
- Farber D. L. (2021). Tissues, not blood, are where immune cells function. Nature, 593(7860), 506–509.
- Szabo, Peter A et al. Longitudinal profiling of respiratory and systemic immune responses reveals myeloid cell-driven lung inflammation in severe COVID-19. Immunity vol. 54,4 (2021): 797-814.e6.
- Cowan, K., Macluskie, G., Finch, M., Palmer, C., Hair, J., Bylesjo, M., Lynagh, S., Brankin, P., McNeil, M., Low, C., Mallinson, D., Gourlay, E. M., Child, H., Cheyne, L., & Bunton, D. C. (2019). Application of pharmacogenomics and bioinformatics to exemplify the utility of human ex vivo organoculture models in the field of precision medicine. PloS one, 14(12), e0226564.




%20(1).png?width=1000&height=562&name=New%20Approach%20Methodologies%20(NAMs)%20(1).png)
.jpg?width=1000&height=562&name=New%20Approach%20Methodologies%20(NAMs).jpg)
.png?width=1000&height=562&name=New%20Approach%20Methodologies%20(NAMs).png)

